Stevie Brown’s ACL Surgery: 63 Minutes to a New Knee
From now until the opening of training camps, The MMQB is running a series of our Greatest Hits from the site’s first year. From September, Jenny Vrentas is in the operating room when surgeons repair Giants safety Stevie Brown's torn ACL.
GULF BREEZE, Fla. — Dressed in cerulean blue scrubs and white rubber boots, the most well-known orthopedic surgeon in America exits Operating Room Number 3 at the Andrews Institute, where athletes from all sports come to have their careers saved. James Andrews has just finished saving another one, that of Giants safety Stevie Brown.
Before he can take a bite of his post-surgery blueberry muffin, Andrews makes a call to Giants team physician Russell Warren. He gets Warren’s voicemail.
“Hey, Russ. Jim Andrews. Stevie Brown’s down here. I just got through doing his ACL.”
Brown had torn the anterior cruciate ligament in his left knee in a preseason game 12 days earlier on one of those all-too-common awkward plants. He commissioned Andrews to replace the small but critical bridge of tissue between the tibia (shin) and femur (thigh) bone that, when torn, instantly ends an athlete’s season.
ACL surgery is ubiquitous in sports. But what do most of us really know about it? Do we know it involves a power drill boring into leg bone? Do we know that so much cleansing saline solution is pumped into the knee during surgery that Andrews wears calf-length all-weather boots in the operating room? Do we know the ligament can be reconstructed—at least in this case—in just 63 minutes?
That’s what happened inside an operating room in northern Florida on Sept. 5. Brown allowed The MMQB behind the scenes to chronicle one of the most critical and intimidating days of an athlete’s career. Andrews and his team of six medical professionals carved, probed, debrided, drilled and screwed inside Brown’s left knee joint—this common surgery nothing short of incredibly complex.
Surgical Observation Room | 8:32 a.m. CDT
Andrews sits on a couch, eating a banana and watching baseball highlights on SportsCenter. He seems relaxed. Why wouldn’t he be? The 71-year-old performs about 500 orthopedic surgeries a year and has done thousands over his 40-plus year career. It was his deft work that enabled Adrian Peterson to return to the field nine months after similar surgery and play at an MVP level in 2012.
Andrews spends Mondays and Wednesdays seeing patients upstairs in one of his five exam rooms. Tuesdays and Thursdays are for surgeries. He often examines patients and then adds them to the next day’s operating schedule, as he has done with Brown, who was told to report this morning by 8 a.m.
Pre-operative Area | 8:49 a.m.
Giants safety Stevie Brown had surgery to repair his left ACL on Sept. 5. Richard Lamour, a fellow at the Andrews Institute, initialed the injured knee to make sure doctors operated on the correct leg.
No breakfast for Brown. The common rule for surgery applies: No food after midnight. Brown treated himself to a burger Wednesday night, making a rare exception to eat red meat given the circumstances.
This is the 26-year-old’s first surgery since he broke his ankle his senior year at Columbus East High, about 40 miles south of Indianapolis. He claims he’s not nervous. Just in case, though, Darin Nye, one of Andrews’ yearlong orthopedic sports medicine fellows, lightens the mood with some college football smack talk to the Michigan man.
“Go Bucks!” Nye, a graduate of Ohio State’s medical school, says cheerfully.
Brown shakes his head side to side and chuckles.
“It’s OK,” he says. “We’ll see at the end of the season.”
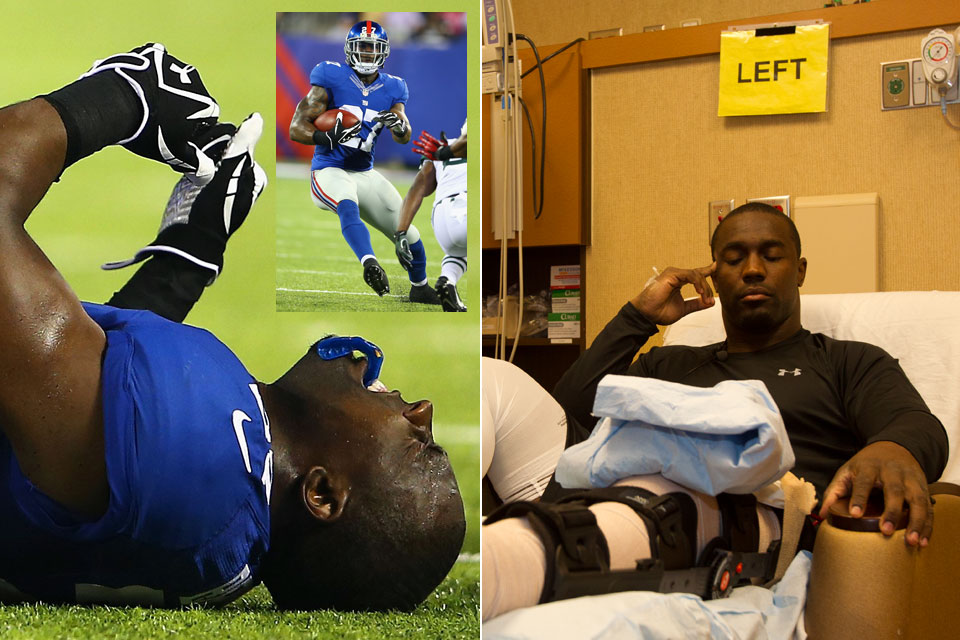
Nye leans over Brown’s bed, checking for a mark just above his left kneecap. Richard Lamour, another doctor who is a fellow with Andrews, signed his initials here with a black permanent marker earlier this morning. This is part of the pre-surgery checklist. A yellow sign with the word LEFT hangs on the wall above Brown’s head, and he will confirm to the staff three separate times that he’s having surgery on this knee before he is taken to the operating room.
Brown crumpled to the turf while returning an interception against the Jets in the third preseason game on Aug. 24.
The left knee is the one Brown grabbed in pain as he tumbled to the MetLife Stadium turf while returning an interception of the Jets’ Geno Smith during the third preseason game. An MRI the next day confirmed the tear, and Brown spent the next several days researching where to have the surgery. Teammate Terrell Thomas, who is back on the field this season after enlisting Andrews for his third ACL operation, was among those who recommended that Brown come here. Brown had flown down two days earlier, though he missed his scheduled connecting flight to Pensacola because he couldn’t walk fast enough on a bad knee between terminals in Atlanta’s sprawling airport.
Brown is prepped for surgery, with an IV hooked to the back of his right hand and a pulse oximeter, to measure oxygen saturation, clipped to his right index finger. A blood-pressure cuff is wrapped around his left biceps, and the leg that is not being operated on—his right one—will stay encased in a tight white compression sleeve to prevent clots from forming during surgery.
Brown is holding his tablet and two phones in the lap of his lavender hospital gown, but he’s already received plenty of good-luck messages. His older sister, Nikki, sits next to his bed as they wait for him to be taken into the operating room.
“Should be going in any minute,” Brown says.
9:52 a.m. | Operating Room Number 3
The last thing Brown remembers before surgery is a doctor leaning over him, telling him to take a few deep breaths.
About 15 minutes before his ACL operation begins, Brown is placed under general anesthesia. His left leg has also been numbed with a nerve block, a local anesthetic injected through a needle near the femoral nerve with the aid of an ultrasound, performed by director of anesthesia Gregory Hickman.
Nikki starts wandering through the facility’s lobby and parking lot, carrying Stevie’s tablet and phones in her oversized black clutch. She is a registered nurse at a medical center in Houston, in the orthopedics department no less, but her little brother’s surgery is one she simply can’t watch.
10:10 a.m. | Operating Room Number 3
The extent of Brown's knee damage wasn't known until Dr. James Andrews opened him up two weeks ago.
Brown is asleep on the operating table, his left leg peeking out from a blue surgical sheet. Using a scalpel, Andrews makes his first incision into Brown’s left knee.
The vertical cut is about three inches long. It’s neither messy nor bloody, but rather like everything else in the room: clean, neat, precise. Andrews and the six members of his team inside the room—Nye, another Andrews fellow, two surgical technicians, a circulating nurse and an anesthesiologist—work calmly and in concert. One of the technicians prepares instruments two steps in advance, arranging them on a waist-high tray before she passes them to the operating table. A visiting resident stands several feet back, arms folded, observing.
Brown’s ACL will be replaced with a graft from his patella tendon, which stretches from the kneecap down to the tibia. The two fellows pull back Brown’s skin from the incision with metal retractors, revealing the pinkish-white tissue underneath. Andrews leans over with a harvesting knife, the double blades spaced 11 millimeters apart, which will allow him to slice out a piece exactly this width from the middle third of the tendon. He then uses a tool similar to a chisel to pry out a piece of the kneecap and a piece of the tibia that remain attached to opposite ends of the tendon, bookending the graft.
Andrews handling the patella tendon graft that he inserted into Brown's knee as the new ACL.
The skinny tube of tissue Andrews holds in his left hand a few minutes later—slightly larger than a pinky finger—will allow Brown to play football again.
Andrews wraps his fingers around the graft as he walks to a back table in the operating room and takes a seat. Peering down through his square glasses, he begins shaping the graft. He whittles down the bone plugs at both ends with a bone-gnawing tool called a rongeur, and measures them. Next, he picks up a drill to bore fine-point holes in the plugs, so sutures can be threaded through to act as handles for the graft. Andrews uses a purple pen to mark each end of the graft, then places it in a rectangular white basin.
“This is really important, to put the graft aside,” says Lamour, the Andrews fellow who is watching the surgery through the observation window. “Everybody knows not to touch it, and there is going to be one person designated to bring the graft from the back table. Because if that hits the ground, that’s a problem.”
Andrews returns to the operating table and completes the row of stitches that close together the outer two thirds of Brown’s patella tendon. The skin around the incision in Brown’s knee looks abnormal—wrinkly and yellow-tinged—because it’s covered with an iodine wrap that helps keep the surrounding area sterile.
10:32 a.m. | Operating Room Number 3
While the ACL injury made Brown question his NFL future, it was just another day at the office for the 71-year-old Andrews (second from r.), who performs about 500 orthopedic surgeries a year.
This is the part Andrews calls “putting all the cards on the table.” An arthroscope will allow him to see inside Brown’s injured knee for the first time, exposing the full extent of the damage, and then aid him in fixing it.
Six black-and-white images of Brown’s left knee, the X-Rays and MRIs taken in New York after his injury, are projected on a screen above the operating table, but the arthroscope’s small lens and light source, attached to a video camera, will give a clearer picture. The instrument, about the size of a drinking straw, is shimmied into the knee joint through the upper corner of the initial incision.
After about 20 seconds a magnified and illuminated view inside the knee is shown on three high-definition screens in the operating room. The picture is cloudy at first, obscured by knee fluid that has the consistency of egg whites and leftover blood from the ACL tear. Liters of sterile saline solution are pumped through a blue tube attached to the arthroscope, cleaning out the joint.
The skinny tube of tissue Andrews holds in his left hand—slightly larger than a pinky finger—will allow Brown to play football again. "If that hits the ground," Lamour says, "that's a problem."
Brown’s MRI results indicated an unusual ACL tear, one more typically seen in children, in which the ligament pulls off the shin bone instead of tearing off the femur or in the middle of the ligament. Sometimes this means the ligament can be simply reattached. But the scope shows frayed and loose white fibers, damage to the substance of Brown’s ACL. Andrews opts for the safest and strongest fix, which is to proceed with the standard patella tendon graft replacement.
Andrews stands at the base of the operating table, his right hand holding the top of the arthroscope and his stare locked on the TV screen. Each instrument used to fix the knee joint will be inserted one at a time through another small portal in the original knee incision. Right now Andrews’ left hand is holding the handle of a mechanical shaver plunged into the knee joint to bite away and suction out the injured tissue. A technician switches the tip of the instrument, and Andrews continues, now burrowing into the bottom of the femur to create space for the graft.
The anatomy of the knee.
Inside the knee joint, there is no margin for a navigation error. But Andrews discovers good news about Brown’s injury: It is an isolated ACL tear. None of the other ligaments are damaged, and Andrews finds an intact meniscus while probing with a spinal needle. There are also no wear patterns on the bone surfaces.
The techniques used to replace the ACL with the graft, and put the knee back together, are akin to carpentry. This includes the use of a power drill, one that makes the same whirring noise you’d hear in a workshop. It takes a few minutes to drill a tunnel through each bone, first the tibia and then up through the femur. The tunnel is exactly 11 millimeters in diameter, to match the patella tendon graft.
Saline solution is suddenly rushing out of Brown’s knee from the hole that has been drilled in the bone, running like a faucet down his shin and onto the floor. This, Lamour says, “is why we all wear these crazy boots.”
Hovering over the operating table, Andrews signals for the designated technician to bring him the graft from the back table, which he removes from the basin with his left hand. Nye threads the long blue sutures hanging off the graft through the eyelet of a large pin, which runs through Brown’s knee and pokes out of his thigh. A technician yanks from the top, and the graft is pulled through the tunnel they drilled. Andrews nudges the graft into position, using the scope and another instrument slid inside the knee.
“It’s perfect,” Lamour says. The graft is straight and the correct length, and its purple-marked ends are aligned with the designated attachment sites to the thigh and shin bones. Now it just needs to be secured in place.
Andrews gives two thumbs up before stepping out of the operating room to call the Giants’ team doctor with an update.
In about three months’ time, the bone plugs at the ends of the graft will have fused to the femur and tibia, making the knee strong and sturdy. But to begin the healing, the plugs are affixed to the bones with screws. Andrews inserts a metal probe to check the tension of the new ligament, while one of the other doctors bends and flexes Brown’s leg.
After about 30 seconds, Andrews puts the probe down and walks toward the observation window, nodding. Brown’s knee still needs to be evacuated of excess fluid, stitched back up and cleaned. He’ll also receive a platelet-rich plasma injection to accelerate healing. But the surgery is essentially complete.
Andrews flashes a double thumbs-up. A few seconds later, a nurse brings Nikki into the observation room. Andrews waves heartily and gives her another thumbs-up. At 11:13 a.m., Brown’s knee is officially fixed.
11:15 a.m. | Surgical Observation Room
Andrews finishes his voicemail to the Giants’ team physician.
“I put a nice 11-millimeter graft in. Everything else was normal,” Andrews tells Warren, who is also an orthopedic surgeon. “I apologize for him being down here; I don’t need to be doing any of your guys. It always makes me feel bad. Anyway, we got him fixed good. If you need anything, holler at me. I’m on my cell phone all day. Hope you all are doing well. And beat up on those Cowboys Sunday night.”
Now for that blueberry muffin. Andrews has worked up an appetite putting Stevie Brown’s knee back together.
"The easy part is done," Nye tells Brown. "Now starts the hard part."
ACL surgeries are routine for Andrews, but his experience tells him never to take anything for granted. Each injury is different, and the success of his work isn’t measured on the day of the operation.
“You don’t pat yourself on the back and start jumping up and down because you are finished with the surgery, because that’s just part of your responsibility,” Andrews says. “I worry about patients I operate on all the way through their first year back playing football. I try to follow them for a long time making sure they are healthy. It’s not a time to celebrate; it’s a time to move forward and go to the next step to get him well.”
1:19 p.m. | Recovery Room
Though his knee was braced and covered with ice, Brown couldn't feel a thing in the recovery room.
Still a little groggy, Brown sits in a tan recliner, with a second printed sign hanging over his head: STEPHEN BROWN. DR. ANDREWS.
Andrews had given Brown the three words he was hoping to hear—“everything went fine”—which triggered an immediate sense of relief. Now he’s trying to wrap his head around how large his left leg looks, wrapped in gauze and locked in a black knee brace, with an ice pack resting on top.
“This ice is sitting here,” he tells his sister, “but I don’t feel it.”
“You’re not going to feel anything for a while,” Nikki assures him. She worked the night shift in Houston on Tuesday and made the seven-hour drive late Wednesday so she could take care of her brother for the first few days of his recovery.
Hickman inserted a catheter just above Brown’s knee post-surgery, connected to a pump with a numbing agent. This will dull the pain in the knee joint for four days, without numbing the quadriceps muscle, so Brown can begin physical therapy the next morning. Hickman says the Andrews Institute has seen this technique, which is not yet widely used, speed up recoveries by helping patients regain strength in their quadriceps two to three months earlier.
Doctors and nurses pop in and out of the recovery room, giving Brown instructions (turn on the pain pump to level four at bedtime), benchmarks (the first goal is to achieve full extension of the knee) and advice (a successful return is based one-third on the surgery, one-third on the rehab and one-third on your attitude).
Keeping a positive outlook has never been an issue for Brown. The former seventh-round pick had stints with three NFL teams in his first two seasons in the league before the Giants signed him in 2012 to be a special-teams player. Instead, he was a bright spot for the defense, snatching eight interceptions and a starting job.
Brown's contract expires at the end of the season, but he can only focus on immediate tasks like getting in the car and going to rehab, which one Andrews fellow called "the hard part" of tearing an ACL.
Brown’s injury, though, is the most significant hurdle so far in his professional career. As a restricted free agent this past offseason, he signed a one-year tender worth roughly $2 million. He’ll be fully compensated while on IR, but his future is uncertain. He hopes he can stay with the Giants next season, but he must push such concerns to the back of his mind. First things first: He will stay in Florida for one month, with the Giants offering to pay for his first two weeks of lodging, and start his rehabilitation under the care of the Andrews Institute.
At 2:03 p.m., two nurses wheel Brown out to Nikki’s car.
“The easy part is done,” Nye tells him. “Now starts the hard part.”
“Yep,” Brown says. “Definitely ready for it.”
8:13 p.m. | Hilton Pensacola Beach
On the television in Brown’s beachfront hotel suite (he got upgraded), the 2013 NFL season kicks off in Denver. He watches every play of the Broncos’ blowout win over the Ravens, mainly because he can’t get comfortable enough with his bulky knee brace to fall asleep. Brown is on a new schedule now, one in which games are background noise. His own kickoff will be at 9 the next morning. That’s his first session of physical therapy, when his road back to the NFL begins in earnest.
“I’m excited, actually,” Brown says. “It’s unfortunate this happened. But now that the surgery happened, I can put the incident behind me, and I can look forward to next year. That’s how I’m going to approach it. Every time I come into rehab, it’s just marking off the days till next season.”
More on ACL Injuries
Can a Soccer Doctor Save NFL Players' Knees?
The Business of Getting Better—and the Best: Why Team Doctors Are Being Used Less and Less